Laurie Anne Walden, DVM Photo by Hal Gatewood on Unsplash Photo by Hal Gatewood on Unsplash Over-the-counter (nonprescription) pain medications can cause serious problems for dogs and cats. Because these medications don’t need a prescription and are used for children as well as adults, some pet owners mistakenly believe that they’re safe for animals too. But dogs and cats don’t process these drugs the same way as humans. If your pet has signs of pain, call your veterinarian instead of giving your pet something from your medicine cabinet. Prescription pain medications developed specifically for dogs and cats are safer and more effective for them than over-the-counter human medications. In any case, animals that have a level of pain high enough to be obvious to a human need to see a veterinarian. Nonsteroidal Anti-Inflammatory Drugs (Aspirin, Ibuprofen, Naproxen) The most common human nonsteroidal anti-inflammatory drugs (NSAIDs) available without a prescription are aspirin, ibuprofen, and naproxen. Some brand names are Advil, Aleve, Ascriptin, Bayer, Bufferin, Ecotrin, Midol, and Motrin. In animals, NSAIDs can cause these problems:
NSAIDs reduce inflammation by blocking the activity of cyclooxygenase (COX) enzymes, which are responsible for prostaglandin production. Prostaglandins are hormone-like substances with many functions; they’re involved in the inflammatory response and also protect the stomach lining and maintain blood flow to the kidneys. Because NSAIDs decrease prostaglandin levels, these medications decrease inflammation and pain. However, the lower prostaglandin levels can also cause serious adverse effects like stomach ulcers and kidney damage. Some newer NSAIDs target specific COX enzymes and prostaglandins that are less likely to affect the stomach and kidneys. Several NSAIDs have been approved for use in dogs, and a few are available for cats. Examples are carprofen, grapiprant, deracoxib, and robenacoxib. These species-specific drugs are available only by prescription from a veterinarian and are less likely than human NSAIDs to cause adverse effects in dogs and cats. Animals receiving prescription NSAIDs need regular examinations and bloodwork to monitor kidney and liver function. Acetaminophen Brands containing acetaminophen include Tylenol, Panadol, Excedrin, and Midol. Some pain relievers labeled “complete” or “dual action” contain acetaminophen plus aspirin or ibuprofen. Acetaminophen is also called paracetamol. Acetaminophen is highly toxic and often fatal to cats. Acetaminophen is also potentially toxic to dogs, but it can be used in dogs with caution and veterinary oversight. In humans and dogs, acetaminophen is broken down mainly in the liver through a process called glucuronidation. A toxic dose of acetaminophen in a human or a dog damages liver cells and causes liver failure. Cats don’t have the enzymes needed for glucuronidation, so their bodies break down acetaminophen through a different process called sulfation. The sulfation process in cats creates products that react to hemoglobin, the substance within red blood cells that carries oxygen throughout the body. In cats, acetaminophen exposure causes anemia and life-threatening oxygen deficiency. Cats that swallow acetaminophen are less likely than dogs to develop liver failure because they usually die of oxygen deficiency before the liver has a chance to fail. An antidote to acetaminophen (N-acetylcysteine) is available, so dogs and even cats with acetaminophen poisoning can recover if they are treated immediately at an emergency veterinary clinic. For More Information Get the Facts About Pain Relievers for Pets (US Food and Drug Administration): https://www.fda.gov/animal-veterinary/animal-health-literacy/get-facts-about-pain-relievers-pets Image source: https://unsplash.com/photos/round-white-pills-iPl3q-gEGzY Laurie Anne Walden, DVM Photo by Anya Prygunova on Unsplash Photo by Anya Prygunova on Unsplash In recent years, monoclonal antibodies have been approved to treat some common medical conditions in animals:
More monoclonal antibodies are likely to become available for dogs and cats. Monoclonal antibodies are used in humans to treat infections, autoimmune disorders, cancer, and other conditions, and they’re being investigated for similar uses in dogs and cats. How Monoclonal Antibodies Work Monoclonal antibodies are in a therapy class called biologics, meaning therapies made from living sources like animal cells, plant cells, or microorganisms. Biologics are large molecules that interact with receptors on the outer surfaces of cells; they don’t enter cells. In contrast, most traditional drugs are small molecules that work inside cells. Monoclonal antibodies are similar to the natural antibodies produced by the immune system. When the immune system detects an antigen, different immune cells release lots of different antibodies that tag different sites on that antigen. (An antigen is anything that triggers an immune response.) Once the antibodies have tagged the antigen, other components of the immune system arrive to destroy it. Monoclonal antibodies are cloned in a laboratory from just one antibody made by one type of immune cell (mono means “one”). They tag only a single site on an antigen. Monoclonal antibody therapy can be very precise because it directs the immune response to a narrow target. In addition to tagging invaders like viruses, monoclonal antibodies can be engineered to tag a receptor on an animal’s own cells. The monoclonal antibodies that relieve pain in dogs and cats, for example, block production of a protein that’s partly responsible for the pain sensation. After monoclonal antibodies have activated the immune system, they’re broken down in the body the same way that natural antibodies are. Unlike small-molecule drugs that enter an animal’s cells, they aren’t cleared through the liver or kidneys. Administration Monoclonal antibodies are given by injection at a veterinary clinic. They can’t be given by mouth because they’re proteins and would be destroyed by digestion. Their effect lasts a few weeks (4-8 weeks for Cytopoint, 4 weeks for Solensia and Librela). These therapies are species specific: monoclonal antibodies for dogs work only for dogs, not for cats. Benefits The monoclonal antibodies that are available for dogs and cats generally work well for their approved uses. They are less likely than some traditional drugs to cause adverse effects because they have a narrow target of action and don’t enter cells. Because they are not cleared through the liver or kidneys, they can be safer than other drugs for animals with liver or kidney disease. Injections given every few weeks might be more convenient for pet owners than pills given multiple times a day, especially if their pets resist oral medication. Adverse Effects Monoclonal antibodies have fewer adverse effects than many traditional drugs. An antibody injection can cause an allergic reaction, although this is rare. Manufacturers might recommend precautions for individual monoclonal antibody products. Image source: https://unsplash.com/photos/a-dog-wearing-a-baseball-glove-E3K7xyAvQ8M  Cats don’t often show obvious signs of pain (at least not obvious to people). Because cats don’t speak human, we have to learn to speak cat—that is, read their behavior cues and body language—to know when they’re hurting and need help. September is Animal Pain Awareness Month, so this article highlights 2 tools used to evaluate pain in cats. Cat owners and veterinarians can use the Feline Musculoskeletal Pain Index (FMPI) to identify signs of joint pain in cats. The Feline Grimace Scale uses changes in cats’ facial expressions to help veterinarians assess the need for pain relief in hospitalized cats. If you think your cat is in pain, contact your veterinarian. Never give a cat any pain medication unless your veterinarian has specifically recommended it. Many over-the-counter and prescription pain medications for humans and dogs are dangerous for cats. Feline Musculoskeletal Pain Index Arthritis is very common in senior cats and can also affect young cats. Other joint and tendon disorders also cause chronic (long-term) pain in cats. These conditions are notoriously difficult to diagnose in cats by physical examination alone; cats don’t tend to cooperate during orthopedic exams. However, chronic pain causes changes in behavior and mobility that we can observe and track over time. Researchers at NCSU College of Veterinary Medicine developed the FMPI to help cat owners and veterinarians diagnose and monitor chronic pain caused by joint disorders. This tool has been clinically validated, meaning that it’s accurate and reliable. The FMPI is a questionnaire for cat owners. In the questionnaire, owners rank their cat’s ability to perform normal activities like these:
Each item is scored, and the total score indicates the cat’s level of impairment. After a cat starts treatment, the FMPI can be used to evaluate whether the cat’s pain is decreasing over time. You can find more information about the FMPI at its website: https://painfreecats.org/. Feline Grimace Scale Grimace scales are used to assess pain in a number of animal species. These scales evaluate changes in facial expression caused by tension in specific facial muscles in response to pain. Researchers at the University of Montreal developed the Feline Grimace Scale to help veterinarians detect acute (short-term) medical, surgical, or dental pain in cats in the hospital. This scale, like the FMPI, has been clinically validated. The Feline Grimace Scale includes 5 facial action units that reflect levels of pain:
Each facial action unit is scored, and the total score indicates the cat’s level of pain. A score above a certain point suggests that a cat needs pain medication. The scale is also used to monitor response to pain medication. More information, including illustrations of the different facial expressions, is available at the Feline Grimace Scale website: https://www.felinegrimacescale.com/. Photo by Yerlin Matu Laurie Anne Walden, DVM 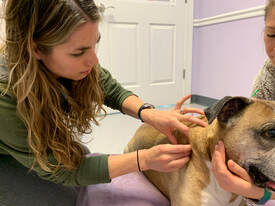 Dr Ponce and Rocky Dr Ponce and Rocky Acupuncture, the technique of stimulating points on the body by inserting tiny needles through the skin, is being used more frequently to treat animals. Most scientific studies of acupuncture have been conducted in humans. However, the existing evidence in animals led the American Animal Hospital Association and American Association of Feline Practitioners to endorse acupuncture as a treatment option for chronic pain.[1] Anna Ponce, DVM, and I recently sat down to chat about acupuncture in pets. Dr Ponce provides acupuncture services for dogs and cats and has completed the coursework and examination requirements for certification in veterinary acupuncture. (Interview has been edited for length and flow.) LAW: How did you decide to start doing acupuncture? AP: My biggest push to learn acupuncture was having geriatric cats come in with arthritis. Some of them have kidney disease, and there is just no good long-term arthritis medication for these cats. Acupuncture is one of the modalities that has been mentioned, so I decided to explore that avenue and see what I could do to help arthritic cats. And that really opened my eyes to so much more that can be done with acupuncture. What conditions do you think acupuncture helps the most? It can really help with any condition: heart disease, kidney disease, coughing, behavioral issues, anxiety. But I think what we know it most commonly for is arthritis. Which patients do you recommend it for, and how does it help them? For example, this morning I recommended it for a dog that has arthritis in her knees, elbows, back, and hips. She’s had x-rays, so we know arthritis is there. It took a long time to get her on the right combination of drugs to be comfortable, but she still has off days and I absolutely think she would benefit from acupuncture. Acupuncture has local effects like decreasing inflammation and pain, and it also helps get the body back in balance. Chronic issues are obviously going to take more time. Acupuncture is not going to make these issues disappear. It doesn’t miraculously make degenerative joint disease return to normal, but it definitely helps the pain and inflammation. [It helps the body release] serotonin, endogenous opioids, and beta endorphins. In my opinion, there’s not a pet that can’t benefit from acupuncture, even if it’s as a preventive measure. When would you not recommend it? I wouldn’t not recommend it for just about any patient, but the biggest consideration is whether the patient will tolerate acupuncture. Some dogs and cats fall asleep, they snore, they love their acupuncture, they look forward to it, they’re very relaxed. And then some patients are just not going to tolerate having needles placed in them. You would not want to put a needle through infected skin. You wouldn’t want to put a needle in a tumor because it would increase blood supply to that area. Certain points are contraindicated in pregnant dogs to avoid inducing labor. And you would not do electroacupuncture [delivery of electrical current through acupuncture needles] in a dog with seizures. But other than that it’s very safe. There’s really not a patient that I would say should not get it. It’s a matter of whether they tolerate it, which I feel most of them do. How do cats handle it? I have one cat patient who is very good for his acupuncture. He tells me when he’s had enough needles, so he dictates how many needles he gets. When he starts to meow a little bit and get a little twitchy, we’ve reached our limit, and then he walks into his carrier, lies down, and rests there [with the needles inserted]. Another cat that I treated really enjoyed it and just lay there the entire time, comfortable. Can you describe a typical acupuncture session? We use very tiny sterile needles that go in acupuncture points throughout the body. The needles are even smaller than insulin needles. I do a traditional Chinese exam along with my Western exam, make my traditional Chinese diagnosis, and pick acupuncture points based on that. A session might include 5 to 40 needles, depending on what I’m treating; it’s normally 10 to 20 needles. The time patients sit with the needles inserted could be anywhere from 10 to 40 minutes. Placement of the needles is based on meridians through which qi (chi), or energy, flows and where acupuncture points are located. The strongest points tend to be on the limbs, but those can also be more tender points for dogs and cats. So we often use more points on the back because they’re easier to access and they tend to not be quite as sensitive as the points on the limbs. When a needle’s inserted it causes a de-qi response, essentially a tingling or warming sensation, and sometimes a muscle twitch. I also use different modalities. Dry needling is insertion of the tiny needles. In electroacupuncture, we hook up electrodes to get higher stimulation. In aquapuncture, we inject vitamin B12 under the skin at acupuncture points to get a longer effect. How do you integrate acupuncture with Western medicine? I believe that they complement one another. I think that acupuncture can benefit the patient in ways that Western medicine can’t, especially with end-of-life comfort and pain relief. I definitely wouldn’t throw out Western diagnostics. Bloodwork and x-rays are very important and can help tailor your acupuncture treatment. I think the best type of medicine is an integrative approach, having them work together. Would you describe your acupuncture training? You have to be a licensed veterinarian to practice acupuncture [in animals], but you do not have to have a certification in acupuncture to practice it. Being certified shows that you have gone through the training and that you know what you’re doing. I took a 6-month course through the Chi Institute [of Traditional Chinese Veterinary Medicine] in Florida. The course is 150 credit hours in 5 sessions: 2 online lecture sessions and 3 on-site sessions including lectures and a hands-on lab. After you complete the sessions you take a 200-question written exam and a practical exam. The final requirements for certification are a 30-hour internship with a certified veterinary acupuncturist and submission of a case study of a patient that you have followed for at least 3 months. I’ve done all of the coursework and the test. Once my internship hours are finished and my case study has been approved, I’ll get my certification. Reference 1. Epstein ME, Rodan I, Griffenhagen G, et al. 2015 AAHA/AAFP pain management guidelines for dogs and cats. J Feline Med Surg. 2015;17(3):251-272. Laurie Anne Walden, DVM  In cats and dogs, chronic (long-term) pain causes subtle behavior changes that can be mistaken for normal effects of aging. Pain can also cause unwanted behaviors like house soiling. Don’t assume that changes in behavior, activity, or mood result from aging, anxiety, or human emotions like resentment or anger. Your pet could be in pain instead. Arthritis is one of the most common causes of chronic pain in older animals but can go undetected, especially in animals like cats that are biologically programmed to hide their pain. Signs of acute pain (caused by injury) are easier to spot. Whatever the cause of your pet’s pain, recognizing the signs is the first step to helping your pet feel better. If you think your pet may be in pain, consult a veterinarian. Never treat an animal’s pain with over-the-counter medications, herbs, supplements, or other remedies without checking with your veterinarian first. Many over-the-counter pain remedies, like acetaminophen (Tylenol), ibuprofen (Advil and Motrin), and naproxen (Aleve), are toxic or even fatal to dogs and cats. Your veterinarian can suggest safer and more effective measures for your pet. Signs of Pain in Cats
Signs of Pain in Dogs
More Resources 15 Signs of Pain in Dogs (PDF, American Animal Hospital Association): https://www.aaha.org/globalassets/02-guidelines/pain-management/painmgmt_15signs.pdf How Do I Know if My Cat Is in Pain? (American Association of Feline Practitioners): https://catfriendly.com/feline-diseases/signs-symptoms/know-cat-pain/ How to Tell if Your Dog Is in Pain (PDF, American Animal Hospital Association): https://www.aaha.org/globalassets/02-guidelines/pain-management/painmanagement_dogs_web.pdf Photo by Priscilla Du Preez |
AuthorLaurie Anne Walden, DVM Categories
All
Archives
June 2024
The contents of this blog are for information only and should not substitute for advice from a veterinarian who has examined the animal. All blog content is copyrighted by Mallard Creek Animal Hospital and may not be copied, reproduced, transmitted, or distributed without permission.
|
- Home
- About
- Our Services
- Our Team
-
Client Education Center
- AKC: Spaying and Neutering your Puppy
- Animal Poison Control
- ASPCA Poisonous Plants
- AVMA: Spaying and Neutering your pet
- Biting Puppies
- Boarding Your Dog
- Caring for the Senior Cat
- Cats and Claws
- FDA warning - Bone treats
- Force Free Alliance of Charlotte Trainers
- Getting your Cat to the Vet - AAFP
- Holiday Hazards
- How To Feed Cats for Good Health
- How to Get the Most Out of your Annual Exam
- Indoor Cat Initiative - OSU
- Introducing Your Dog to Your Baby
- Moving Your Cat to a New Home
- Muzzle Training
- Osteoarthritis Checklist for Cats
- What To Do When You Find a Stray
- Our Online Store
- Dr. Walden's Blog
- Client Center
- Contact
- Cat Enrichment Month 2024
|
Office Hours
Monday through Friday 7:30 am to 6:00 pm
|
Mallard Creek Animal Hospital
2110 Ben Craig Dr. Suite 100
|
Site powered by Weebly. Managed by IDEXX Laboratories

 RSS Feed
RSS Feed