Laurie Anne Walden, DVM Photo by Madalyn Cox on Unsplash Photo by Madalyn Cox on Unsplash Environmental enrichment means modifying an animal’s living space to encourage physical activity and allow the animal to engage in behaviors that are natural for its species. For indoor pets especially, environmental enrichment improves physical and mental health and can reduce behavior problems. Dogs and cats with mobility problems need environmental modification for accessibility and mental stimulation. Pets have mobility limitations for a variety of reasons:
Household Modifications and Physical Activity Cover hard floors with nonslip mats or rugs. Consider using lots of small washable mats instead of large rugs for easier cleaning if your pet urinates or defecates on the floor (common in animals with medical problems, mobility limitations, or cognitive decline). Be sure to have a nonslip surface in front of your pet’s food and water bowls. Use steps and ramps. Think of all the places your pet likes to be that are not the floor—bed, sofa, cat tree (climbing structure), window seat, and so forth—and make sure your pet can get up and down without jumping. You might need to train your pet to use steps and ramps by leading them with treats. Cats need to scratch for claw health and their mental health (it’s normal species behavior). Reaching and stretching can be difficult for cats with arthritis, so offer your cat horizontal as well as vertical scratching surfaces. Ask your veterinarian about exercise that’s appropriate for your pet. Depending on the medical condition, your pet might benefit from controlled gentle exercise. Some veterinary facilities have physical rehabilitation equipment like underwater treadmills. Toileting Difficulty reaching the toileting area causes anxiety for animals. For cats, put low-sided litter boxes on every floor of the house in quiet, accessible areas. Cats tend to be most comfortable toileting in big open boxes (at least 1.5 times the length of the cat, not including the tail). A large plastic storage bin makes a great litter box; cut an opening on one side so your cat can walk in and out easily. Dogs with new mobility problems or cognitive decline might not give you their usual cues that they need to go out. If your dog or cat starts having toileting accidents indoors, make a veterinary appointment to check for a medical reason. If no medical cause is found, your pet might be having trouble getting outside or to the litter box. Mental Stimulation Engage your pet’s senses: use toys with different odors, textures, and sounds. Puzzle feeders and treat-dispensing toys engage the brain and encourage physical activity. Teach your old dog or cat new tricks. Use positive reinforcement to train new behaviors that don’t require a lot of movement (like touching their nose to your hand). For dogs with mobility problems, walks aren’t really about walking. Just seeing and smelling the outdoors is valuable mental enrichment for dogs. Take your dog out on a harness and forget about actually getting anywhere; be patient and let him sniff and wander at his own pace. If your dog can’t walk easily, carry him or use a wagon. Give your cat a soft seat by a window if possible. Your cat might also enjoy cat-friendly videos. For More Ideas Home modifications. International Cat Care. 2024. Accessed June 18, 2024. https://icatcare.org/app/uploads/2024/03/Changes-to-the-home-environment_ISFM-caregiver-guide_FINAL.pdf Sueda K, Cho J. Environmental enrichment for senior dogs and cats. Clinician’s Brief. December 2017. Accessed June 18, 2024. https://www.cliniciansbrief.com/article/environmental-enrichment-senior-dogs-cats Image source: https://unsplash.com/photos/black-cat-on-white-cat-tree-X7OokuRyvCI Laurie Anne Walden, DVM Photo by Kanashi on Unsplash Photo by Kanashi on Unsplash Vestibular disorders cause problems with balance and coordination. Animals with vestibular disorders typically have a head tilt along with stumbling, walking in circles, and possibly vomiting. Vestibular problems that start suddenly can look scary to pet owners. The signs can be mistaken for stroke. Some conditions that cause vestibular problems are serious, even life-threatening; others are relatively minor. One of the most common vestibular disorders in dogs is a benign condition called idiopathic vestibular syndrome (idiopathic means “of unknown cause”). This condition is not serious and gets better on its own with time. Idiopathic vestibular syndrome most often affects senior dogs, so in dogs it’s also known as old dog vestibular disease. Cats can also develop idiopathic vestibular syndrome. Causes The vestibular system includes the brainstem, cerebellum (part of the brain), inner ear, and nerves that conduct signals between the inner ear and brain. Anything that affects any part of this system can cause vestibular signs. Vestibular disorders are either central (related to the brainstem and cerebellum) or peripheral (related to the inner ear and surrounding nerves). Central vestibular disorders are usually much more worrisome than peripheral vestibular disorders. Idiopathic vestibular syndrome is a peripheral vestibular disorder. The exact cause in dogs isn’t known. Similar conditions in humans are caused by inflammation of the inner ear or surrounding nerves, viral infections, and benign positional vertigo (an inner ear problem). These same causes are possible but not proven in dogs. Some of the other causes of vestibular disease in animals are deep ear infections (common), cancer, drug adverse effects, toxins, systemic disorders like hypothyroidism, meningitis, and other neurologic disorders. Signs These are the typical signs of a vestibular disorder:
Idiopathic vestibular syndrome usually affects older dogs and cats. It begins suddenly and then starts to improve within a few days. The signs are most pronounced on the first day and don’t get worse with time. In most animals, the signs disappear after a couple of weeks, although the head tilt can last much longer. Other diseases that affect the vestibular system cause signs of their own. For example, a central vestibular disorder might cause seizures or changes in consciousness. Vestibular signs that get worse with time are a signal that the animal has something other than idiopathic vestibular syndrome. Diagnosis Idiopathic vestibular syndrome is a diagnosis of exclusion: it’s diagnosed after other possibilities are ruled out. Diagnosis begins with a neurologic examination, eye and ear examinations, baseline bloodwork, and usually a thyroid function test and urinalysis. Depending on the results, the animal might need referral to a veterinary neurologist and advanced tests like magnetic resonance imaging of the head or cerebrospinal fluid analysis. Treatment For idiopathic vestibular syndrome, the goal of treatment is to make the patient comfortable until the condition resolves on its own. Most animals receive prescription antinausea medication; some also need appetite stimulants or fluid therapy. Home care includes making sure they can eat and drink and protecting them from falling down steps or bumping into things like furniture corners. Physical therapy and postural maneuvers that are used to help people with vertigo aren’t commonly used in animals. Prognosis Most animals with idiopathic vestibular syndrome recover completely, although some have a permanent head tilt afterward. Some animals have more vestibular episodes later on. For vestibular signs that aren’t caused by idiopathic vestibular syndrome, the prognosis depends on whether the cause is treatable. Sources
Image source: https://unsplash.com/photos/brown-and-black-german-shepherd-Xy7SLX9zuVM Laurie Anne Walden, DVM Public domain photo by Alan Levine on flickr Public domain photo by Alan Levine on flickr Palliative care and end-of-life hospice care for animals focus on improving quality of life, not curing disease. The decision to begin these types of care can be difficult for pet owners. Whether palliative care is right for an individual pet depends on the needs and capacity of the family as well as the medical needs of the animal, so the decision is specific to each pet and each caregiver. Animals that are candidates for palliative and hospice care typically fall into one of these categories:
Palliative care is treatment that minimizes an animal’s pain and distress (without curing disease) at any time, not just at the end of life. The term hospice care more specifically refers to care near the end of life. Hospice care generally includes palliative care for the animal and support for the human caregivers. The biggest difference between human and animal hospice care is that euthanasia is a legal and humane option for animals. Hospice-assisted natural death is possible for some animals. However, choosing to let pets “die on their own” without any relief of pain and distress is unethical. Some veterinarians are specialists in palliative and hospice care. End-of-life care for animals might involve a team including veterinary staff members, specialists (like grief counselors) to support the humans, and the pet owners themselves. Tips for Pet Owners The American Association of Feline Practitioners recently published hospice and palliative care guidelines for cats and has very helpful suggestions for pet owners (not just cat owners). Here’s a summary; for more details, see the Cat Friendly Homes website.
If you know your pet is nearing the end of life, it can be very helpful to plan in advance for your pet’s death. Options might include euthanasia at your veterinarian’s office, home euthanasia (if available in your location), or hospice-assisted natural death (if appropriate and available for your pet). Ask about the euthanasia procedure and the cremation and burial options. For More Information
Image source: https://www.flickr.com/photos/cogdog/25256183337/ Laurie Anne Walden, DVM Public domain image from pixy.org Public domain image from pixy.org Osteoarthritis is very common in cats but often goes undetected. In most cats, joint pain doesn’t cause obvious signs like limping. Instead, it causes changes in mobility and behavior that can be misinterpreted as normal aging. Cat owners’ recognition of these changes is the first step in diagnosing and relieving joint pain. Cause Osteoarthritis is a chronic disease in which the protective cartilage in a joint wears down. Eventually the bones and other structures in the joint deteriorate, causing pain that worsens over time. Degenerative joint diseases like osteoarthritis can be caused by trauma or by problems with the structure of a joint, but often the cause is not known. Senior cats are by far the most likely to develop osteoarthritis. Younger cats can be affected too. Osteoarthritis in cats most often involves the hips, elbows, knees, and hocks. Cats can also develop degenerative joint disease in the spine. Various studies have shown that between about 60% and 90% of cats have evidence of degenerative joint disease on radiographs (x-ray images).[1-3] Not all of these cats have pain, though, at least not at first. Signs In cats, signs of joint pain are subtle. Cats tend to hide signs of pain. Osteoarthritis often affects joints on both sides of cats’ bodies, so they don’t develop lameness—it’s hard to limp with both front legs or both rear legs at the same time. Signs of osteoarthritis in cats reflect their limited mobility, reduced activities of daily living, and general grumpiness caused by chronic pain:
Diagnosis The most important diagnostic tool is cat owners’ observations of signs of joint pain at home. Treatment is often started just on the basis of behavior changes consistent with pain. Cat owners can use questionnaires like the Feline Musculoskeletal Pain Index (https://painfreecats.org/) to record and score their cats’ signs of pain. These assessment tools help veterinarians diagnose joint pain and are also very useful to track changes over time and monitor response to treatment. Cats with signs of pain should receive a physical examination to be sure the signs are caused by joint or back pain and not by something else. A full orthopedic examination of a cat is challenging (sort of like examining an uncooperative bowl of jello that doesn’t tell you when it hurts and won’t trot on leash), but sometimes an examination reveals joint thickening or other physical changes of osteoarthritis. Radiographs can show evidence of degenerative joint disease but aren’t always needed. The decision to use imaging depends on the individual cat. Treatment Never give a cat pain medication, including nonprescription over-the-counter remedies, without consulting a veterinarian. Some medications that are safe for people and dogs are very dangerous for cats. In cats, joint pain is managed with a combination of nondrug and drug treatments. A multimodal approach (using several strategies) tailored to each cat’s pain level and living conditions is the best way to help relieve chronic pain in cats. Nondrug treatments include weight management, adjunctive therapies like acupuncture, dietary supplements such as glucosamine, and environmental modifications like ramps, steps, soft bedding, and litter boxes with low sides. Drug options are more limited for cats than they are for dogs, but a number of drugs are available. A new injectable treatment for osteoarthritis pain avoids the need to give a cat a pill by mouth.[3] References 1. Lascelles BD, Henry JB 3rd, Brown J, et al. Cross-sectional study of the prevalence of radiographic degenerative joint disease in domesticated cats. Vet Surg. 2010;39(5):535-544. doi:10.1111/j.1532-950X.2010.00708.x 2. Slingerland LI, Hazewinkel HA, Meij BP, Picavet P, Voorhout G. Cross-sectional study of the prevalence and clinical features of osteoarthritis in 100 cats. Vet J. 2011;187(3):304-309. doi:10.1016/j.tvjl.2009.12.014 3. Gruen ME, Myers JAE, Lascelles BDX. Efficacy and safety of an anti-nerve growth factor antibody (frunevetmab) for the treatment of degenerative joint disease-associated chronic pain in cats: a multisite pilot field study. Front Vet Sci. 2021;8:610028. doi:10.3389/fvets.2021.610028 4. Bennett D, Zainal Ariffin SM, Johnston P. Osteoarthritis in the cat: 1. How common is it and how easy to recognise? J Feline Med Surg. 2012;14(1):65-75. doi:10.1177/1098612X11432828 Image source: https://pixy.org/6310117 Laurie Anne Walden, DVM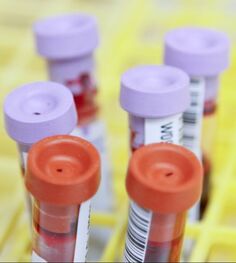 Photo by Daniel Sone, National Cancer Institute. Photo by Daniel Sone, National Cancer Institute. Laboratory testing of blood, urine, and stool samples is routinely done for animals. Abnormalities often show up on lab tests before an animal has obvious symptoms. Even healthy pets need to be tested regularly for parasites. Well-animal tests can detect problems early and help veterinarians track changes over time. These are some of the reasons your veterinarian might recommend lab tests for your pet:
Complete Blood Count A complete blood count measures the number, size, and shape of each type of cell in the blood.
Blood Chemistry Panel Blood chemistry tests measure substances in the blood that indicate changes in organ function or other biological processes. Blood chemistry analysis is run as a panel of many individual tests. A chemistry panel doesn’t always give a diagnosis for a sick animal, but the results can help the veterinarian narrow down the list of possibilities. Veterinary laboratories offer many chemistry panels for different species and diagnostic needs. A small panel that’s sufficient for a young animal before routine surgery might not be appropriate for an ill animal or an older pet. These are a few of the tests commonly included in chemistry panels:
Urinalysis Analysis of the urine includes specific gravity (a measure of urine concentration), pH, chemistry results like glucose and protein levels, and microscopic evaluation for cells, crystals, and bacteria. Urinalysis can reveal urinary tract infection, support a diagnosis of diabetes, and help evaluate the function of the kidneys and other organs. A complete laboratory analysis—especially for a senior pet—should include urinalysis. Parasite Tests Parasites are very common in pet animals (unless they have received regular parasite prevention as recommended by a veterinarian). Many of the parasites that pets carry are contagious to people. At least once a year, pets should have a stool test for intestinal parasites like hookworms and roundworms. Dogs should also have a yearly blood test for heartworm disease. Public domain image source: National Cancer Institute, Daniel Sone (photographer) Laurie Anne Walden, DVM Photo by Tereza Hošková Photo by Tereza Hošková Cancer is most common in older animals but can develop in animals of any age. Cancer can affect almost any part of the body, so the symptoms vary. The earlier cancer is found, the better for the pet. Lumps Lumps and bumps on or under the skin are usually benign, but some are malignant (cancerous). Any lump that’s the size of a pea or larger and present for at least a month, or one that’s rapidly enlarging or changing in appearance, should be checked by a veterinarian. It’s not possible to tell if a lump is cancerous just by the way it feels. Diagnosis usually requires analyzing a sample of the lump under a microscope (see Skin Lumps in Dogs and Cats for more information). Changes in Weight Unexplained or sudden weight loss is a cause for concern. Many diseases, including cancer, can cause weight loss. Unexpected weight gain could also be a sign of cancer if it’s caused by fluid buildup. Decreased Energy Playing less, sleeping more, and moving more slowly could be effects of aging but might be caused by pain or an illness like cancer. Don’t assume that pets (especially seniors) that are slowing down or sleeping a lot are just old or tired; have a veterinarian examine them. Changes in Appetite Cancer often causes a drop in appetite. Reluctance to eat could also be caused by dental disease or other medical problems. Vomiting or Diarrhea Digestive trouble like vomiting and diarrhea is very common in dogs and cats. Vomiting or diarrhea that lasts longer than a few days and doesn’t get better with treatment—especially if the animal also has other symptoms—should be investigated further. Cancer of the digestive tract and many other medical problems can cause long-term vomiting or diarrhea. Signs of Pain Limping, reluctance to move, hunched posture, and other signs of pain could indicate cancer. Bone cancer doesn’t only affect older animals; sometimes it happens in young dogs. Contact your veterinarian if your pet has signs of pain, and never give human pain medication to an animal unless your veterinarian has specifically recommended it. Some human pain medications are toxic to dogs and cats. Coughing or Trouble Breathing Cancer of structures in the chest (lymph nodes, lungs, or heart) and cancer that has spread to the lungs are among the many causes of coughing. Swollen Belly Cancer can cause the belly to swell from fluid buildup, bleeding into the abdomen, or enlargement of abdominal organs like the liver and spleen. Changes in Urine or Stool Changes in urine volume or frequency, blood in the urine or stool, and difficulty passing urine or stool can all potentially be caused by cancer and warrant a veterinary examination. Blood in the stool looks tarry black or bright red depending on the part of the digestive tract it’s from. An inability to pass urine is a medical emergency. Discharge or Drainage Anything oozing or leaking from your pet should be checked by a veterinarian. Cancer is one of the possible causes of unusual discharge from body orifices such as the eyes, nose, mouth, and anus. Foul or Unusual Odor Bad breath is usually caused by dental or periodontal disease but could be a sign of cancer. Cancers inside the mouth and nose can be very hard to see in an animal without sedation. Tumors in other areas of the body can also cause odd odors. Wounds That Don’t Heal A skin sore or wound that doesn’t heal on its own could be a sign of skin disease, infection, or skin cancer. Photo by Tereza Hošková on Unsplash Laurie Anne Walden, DVM 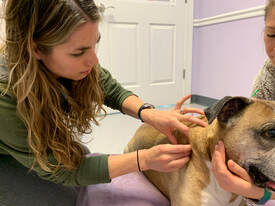 Dr Ponce and Rocky Dr Ponce and Rocky Acupuncture, the technique of stimulating points on the body by inserting tiny needles through the skin, is being used more frequently to treat animals. Most scientific studies of acupuncture have been conducted in humans. However, the existing evidence in animals led the American Animal Hospital Association and American Association of Feline Practitioners to endorse acupuncture as a treatment option for chronic pain.[1] Anna Ponce, DVM, and I recently sat down to chat about acupuncture in pets. Dr Ponce provides acupuncture services for dogs and cats and has completed the coursework and examination requirements for certification in veterinary acupuncture. (Interview has been edited for length and flow.) LAW: How did you decide to start doing acupuncture? AP: My biggest push to learn acupuncture was having geriatric cats come in with arthritis. Some of them have kidney disease, and there is just no good long-term arthritis medication for these cats. Acupuncture is one of the modalities that has been mentioned, so I decided to explore that avenue and see what I could do to help arthritic cats. And that really opened my eyes to so much more that can be done with acupuncture. What conditions do you think acupuncture helps the most? It can really help with any condition: heart disease, kidney disease, coughing, behavioral issues, anxiety. But I think what we know it most commonly for is arthritis. Which patients do you recommend it for, and how does it help them? For example, this morning I recommended it for a dog that has arthritis in her knees, elbows, back, and hips. She’s had x-rays, so we know arthritis is there. It took a long time to get her on the right combination of drugs to be comfortable, but she still has off days and I absolutely think she would benefit from acupuncture. Acupuncture has local effects like decreasing inflammation and pain, and it also helps get the body back in balance. Chronic issues are obviously going to take more time. Acupuncture is not going to make these issues disappear. It doesn’t miraculously make degenerative joint disease return to normal, but it definitely helps the pain and inflammation. [It helps the body release] serotonin, endogenous opioids, and beta endorphins. In my opinion, there’s not a pet that can’t benefit from acupuncture, even if it’s as a preventive measure. When would you not recommend it? I wouldn’t not recommend it for just about any patient, but the biggest consideration is whether the patient will tolerate acupuncture. Some dogs and cats fall asleep, they snore, they love their acupuncture, they look forward to it, they’re very relaxed. And then some patients are just not going to tolerate having needles placed in them. You would not want to put a needle through infected skin. You wouldn’t want to put a needle in a tumor because it would increase blood supply to that area. Certain points are contraindicated in pregnant dogs to avoid inducing labor. And you would not do electroacupuncture [delivery of electrical current through acupuncture needles] in a dog with seizures. But other than that it’s very safe. There’s really not a patient that I would say should not get it. It’s a matter of whether they tolerate it, which I feel most of them do. How do cats handle it? I have one cat patient who is very good for his acupuncture. He tells me when he’s had enough needles, so he dictates how many needles he gets. When he starts to meow a little bit and get a little twitchy, we’ve reached our limit, and then he walks into his carrier, lies down, and rests there [with the needles inserted]. Another cat that I treated really enjoyed it and just lay there the entire time, comfortable. Can you describe a typical acupuncture session? We use very tiny sterile needles that go in acupuncture points throughout the body. The needles are even smaller than insulin needles. I do a traditional Chinese exam along with my Western exam, make my traditional Chinese diagnosis, and pick acupuncture points based on that. A session might include 5 to 40 needles, depending on what I’m treating; it’s normally 10 to 20 needles. The time patients sit with the needles inserted could be anywhere from 10 to 40 minutes. Placement of the needles is based on meridians through which qi (chi), or energy, flows and where acupuncture points are located. The strongest points tend to be on the limbs, but those can also be more tender points for dogs and cats. So we often use more points on the back because they’re easier to access and they tend to not be quite as sensitive as the points on the limbs. When a needle’s inserted it causes a de-qi response, essentially a tingling or warming sensation, and sometimes a muscle twitch. I also use different modalities. Dry needling is insertion of the tiny needles. In electroacupuncture, we hook up electrodes to get higher stimulation. In aquapuncture, we inject vitamin B12 under the skin at acupuncture points to get a longer effect. How do you integrate acupuncture with Western medicine? I believe that they complement one another. I think that acupuncture can benefit the patient in ways that Western medicine can’t, especially with end-of-life comfort and pain relief. I definitely wouldn’t throw out Western diagnostics. Bloodwork and x-rays are very important and can help tailor your acupuncture treatment. I think the best type of medicine is an integrative approach, having them work together. Would you describe your acupuncture training? You have to be a licensed veterinarian to practice acupuncture [in animals], but you do not have to have a certification in acupuncture to practice it. Being certified shows that you have gone through the training and that you know what you’re doing. I took a 6-month course through the Chi Institute [of Traditional Chinese Veterinary Medicine] in Florida. The course is 150 credit hours in 5 sessions: 2 online lecture sessions and 3 on-site sessions including lectures and a hands-on lab. After you complete the sessions you take a 200-question written exam and a practical exam. The final requirements for certification are a 30-hour internship with a certified veterinary acupuncturist and submission of a case study of a patient that you have followed for at least 3 months. I’ve done all of the coursework and the test. Once my internship hours are finished and my case study has been approved, I’ll get my certification. Reference 1. Epstein ME, Rodan I, Griffenhagen G, et al. 2015 AAHA/AAFP pain management guidelines for dogs and cats. J Feline Med Surg. 2015;17(3):251-272. Laurie Anne Walden, DVM  In cats and dogs, chronic (long-term) pain causes subtle behavior changes that can be mistaken for normal effects of aging. Pain can also cause unwanted behaviors like house soiling. Don’t assume that changes in behavior, activity, or mood result from aging, anxiety, or human emotions like resentment or anger. Your pet could be in pain instead. Arthritis is one of the most common causes of chronic pain in older animals but can go undetected, especially in animals like cats that are biologically programmed to hide their pain. Signs of acute pain (caused by injury) are easier to spot. Whatever the cause of your pet’s pain, recognizing the signs is the first step to helping your pet feel better. If you think your pet may be in pain, consult a veterinarian. Never treat an animal’s pain with over-the-counter medications, herbs, supplements, or other remedies without checking with your veterinarian first. Many over-the-counter pain remedies, like acetaminophen (Tylenol), ibuprofen (Advil and Motrin), and naproxen (Aleve), are toxic or even fatal to dogs and cats. Your veterinarian can suggest safer and more effective measures for your pet. Signs of Pain in Cats
Signs of Pain in Dogs
More Resources 15 Signs of Pain in Dogs (PDF, American Animal Hospital Association): https://www.aaha.org/globalassets/02-guidelines/pain-management/painmgmt_15signs.pdf How Do I Know if My Cat Is in Pain? (American Association of Feline Practitioners): https://catfriendly.com/feline-diseases/signs-symptoms/know-cat-pain/ How to Tell if Your Dog Is in Pain (PDF, American Animal Hospital Association): https://www.aaha.org/globalassets/02-guidelines/pain-management/painmanagement_dogs_web.pdf Photo by Priscilla Du Preez Laurie Anne Walden, DVM  Hypertension (high blood pressure) is fairly common in older cats. The condition can cause serious health problems but is treatable. Senior cats and cats with kidney or thyroid disease benefit from routine blood pressure screening. Symptoms High blood pressure is silent; it has no symptoms of its own. But high blood pressure damages organs of the body, causing symptoms that cat owners might notice.
Causes In cats, hypertension is usually caused by another disorder. The most common causes in cats are chronic kidney disease and hyperthyroidism (overactive thyroid). Sometimes high blood pressure in cats seems to develop on its own with no known cause, as can happen in humans. Older cats are more likely than younger cats to have hypertension. Blood pressure measurement Current guidelines recommend measuring blood pressure in cats in these categories [2,4]:
In cats, blood pressure is usually measured with an inflatable cuff similar to the cuffs used in people (but much smaller!). The cuff is placed around a leg or the tail. During the procedure cats can lie down or sit upright, whichever is more comfortable for them. Most operators try to position the cuff at the level of the heart, but forcing a cat to lie down can cause agitation and raise the blood pressure. Blood pressure readings are most accurate in calm cats. You might be asked to wait with your cat in the examination room for a few minutes to give her time to settle down and get comfortable. Consider bringing a cat bed, blanket, or towel from home so your cat can rest on something familiar during the procedure. Blood pressure is typically measured several times during each session to account for variation from motion or anxiety. Cats tend to tolerate the procedure well. A systolic blood pressure below 140 mm Hg is considered normal in cats. (In blood pressure readings like “110/70 mm Hg,” systolic pressure is the first number and diastolic pressure is the second number). A systolic blood pressure of 160 mm Hg or higher indicates hypertension and an increased risk of organ damage.[4] Veterinarians often measure blood pressure on more than 1 clinic visit before making a definite diagnosis of hypertension. Cats’ blood pressures can vary from visit to visit depending on their stress levels. However, signs of organ damage can confirm the diagnosis and justify starting treatment after only 1 measurement session. Cats with hypertension (or at risk for hypertension) should have blood pressure checks every few months. Treatment The goal of treatment is to reduce the risk and extent of organ damage. The underlying problem causing the high blood pressure is treated at the same time. Most cats with hypertension receive daily oral medication. The dose is adjusted as needed after blood pressure rechecks. Medication is usually effective in reducing the blood pressure, especially if the underlying disease is also controlled. References 1. Syme H. Systemic hypertension: World Small Animal Veterinary Association World Congress Proceedings, 2013. VIN website. https://www.vin.com/doc/?id=5709837. Accessed March 25, 2019. 2. Taylor SS, Sparkes AH, Briscoe K, et al. ISFM consensus guidelines on the diagnosis and management of hypertension in cats. J Feline Med Surg. 2017;19(3):288-303. 3. Quinn R. Cardiovascular effects of systemic hypertension in cats. MSPCA Angell website. https://www.mspca.org/angell_services/cardiovascular-effects-of-systemic-hypertension-in-cats/. Accessed March 25, 2019. 4. Acierno MJ, Brown S, Coleman AE, et al. ACVIM consensus statement: guidelines for the identification, evaluation, and management of systemic hypertension in dogs and cats. J Vet Intern Med. 2018;32(6):1803-1822. Photo by Hunt Han Laurie Anne Walden, DVM  Chronic kidney disease is common in cats. It can affect cats at any age but is most common in older cats.[1] The disease has no cure. The goals of treatment are to slow the progression of the disease and maintain a good quality of life for the cat. Functions of the Kidneys The kidneys filter the blood and excrete waste products into the urine. When the kidneys don’t work properly, these waste products accumulate in the body. The kidneys balance the body’s water level by adjusting the urine concentration. Kidney disease impairs the ability to concentrate the urine and retain water in the body, so animals with kidney disease become dehydrated. The kidneys also help regulate blood pressure, red blood cell production, and acid-base balance. Signs of Kidney Disease Kidney disease is already advanced (at least two-thirds of kidney function lost) by the time signs of illness appear. Cats typically have the following signs:
Keep an eye on the size of the urine clumps in your cat’s litter box. Enlarging urine clumps can mean that urine volume is increasing, which is one of the earliest signs of kidney disease. Other disorders (like diabetes) can also increase the urine volume, so larger-than-usual urine clumps warrant a visit to the veterinarian. As chronic kidney disease progresses, the loss of kidney function leads to further problems:
Causes of Kidney Disease Acute kidney injury is a rapid loss of kidney function over hours to days. Some of the many possible causes are toxins, infections, and shock. Depending on the cause and severity, acute kidney damage can sometimes be reversed with treatment. Chronic kidney disease is more common than acute kidney injury in cats. In chronic kidney disease, kidney function gradually decreases over time. The cause is usually not known. The same entities that cause acute kidney injury can lead to chronic kidney failure. Other possible causes are high blood pressure, abnormal kidney development, infection or inflammation of the kidneys, disorders that alter blood flow to the kidneys, and cancer.[2] Diagnostic Tests Tests are used to diagnose kidney disease, assess the stage of the disease, identify metabolic problems caused by the disease, diagnose other disorders (like thyroid disease) that cats with kidney disease sometimes also have, and possibly reveal the cause of the kidney problem. Blood tests and urinalysis (analysis of urine) are typically the first diagnostic tests for cats with suspected kidney disease. Blood pressure measurement, urine culture to test for bacterial infection, and ultrasound or x-ray imaging of the urinary tract are also commonly performed for cats with kidney disorders. Cats with chronic kidney disease benefit from regular testing to monitor disease progression and adjust treatment. In general, these cats should see a veterinarian for blood tests, urinalysis, and blood pressure measurement every 3 to 6 months.[2] The stage and substage of chronic kidney disease are evaluated with specific tests[3]:
Treatment Chronic kidney disease can’t be cured, but it can be managed. The prognosis is variable; some cats can live with the disease for years. If your cat has kidney disease, work with your veterinarian to craft a treatment plan that will give your cat a good quality of life. Treatment strategies are based on the stage of disease and the individual cat’s needs and may include the following[1,4]:
References 1. Sparkes AH, Caney S, Chalhoub S, et al. ISFM consensus guidelines on the diagnosis and management of feline chronic kidney disease. J Feline Med Surg. 2016;18(3):219-239. 2. Brown SA. Renal dysfunction in small animals. Merck Veterinary Manual website. https://www.merckvetmanual.com/urinary-system/noninfectious-diseases-of-the-urinary-system-in-small-animals/renal-dysfunction-in-small-animals. Accessed February 26, 2019. 3. International Renal Interest Society. IRIS staging of CKD. http://www.iris-kidney.com/pdf/IRIS_2017_Staging_of_CKD_09May18.pdf. Updated 2017. Accessed February 26, 2019. 4. International Renal Interest Society. Treatment recommendations for CKD in cats. http://www.iris-kidney.com/pdf/IRIS_2017_CAT_Treatment_Recommendations_09May18.pdf. Updated 2017. Accessed February 26, 2019. Photo by Nicolas Picard on Unsplash |
AuthorLaurie Anne Walden, DVM Categories
All
Archives
June 2024
The contents of this blog are for information only and should not substitute for advice from a veterinarian who has examined the animal. All blog content is copyrighted by Mallard Creek Animal Hospital and may not be copied, reproduced, transmitted, or distributed without permission.
|
- Home
- About
- Our Services
- Our Team
-
Client Education Center
- AKC: Spaying and Neutering your Puppy
- Animal Poison Control
- ASPCA Poisonous Plants
- AVMA: Spaying and Neutering your pet
- Biting Puppies
- Boarding Your Dog
- Caring for the Senior Cat
- Cats and Claws
- FDA warning - Bone treats
- Force Free Alliance of Charlotte Trainers
- Getting your Cat to the Vet - AAFP
- Holiday Hazards
- How To Feed Cats for Good Health
- How to Get the Most Out of your Annual Exam
- Indoor Cat Initiative - OSU
- Introducing Your Dog to Your Baby
- Moving Your Cat to a New Home
- Muzzle Training
- Osteoarthritis Checklist for Cats
- What To Do When You Find a Stray
- Our Online Store
- Dr. Walden's Blog
- Client Center
- Contact
- Cat Enrichment Month 2024
|
Office Hours
Monday through Friday 7:30 am to 6:00 pm
|
Mallard Creek Animal Hospital
2110 Ben Craig Dr. Suite 100
|
Site powered by Weebly. Managed by IDEXX Laboratories

 RSS Feed
RSS Feed