Laurie Anne Walden, DVM Photo by Anna Shvets on Pexels Photo by Anna Shvets on Pexels Home dental care is a crucial part of keeping dogs’ and cats’ mouths healthy. But many pet owners are reluctant to brush their pets' teeth (and brushing is not safe with animals that might bite), so the market is full of products that claim to clean teeth or freshen breath without brushing. Some home dental care products work pretty well, some don’t work at all, and a few pose safety risks for pets. Here’s how to choose dental products for your pet. The Point of Home Dental Care The goal of cleaning your pet’s teeth at home is to remove plaque. Plaque, a sticky biofilm that contains millions of bacteria, attaches to tooth surfaces. Dental disease in dogs and cats is caused by plaque under and at the edges of the gums, not by tartar (hardened plaque) that you can see on tooth surfaces. Like humans, pets need a combination of professional dental cleanings and home dental care. Home dental products can’t remove tartar or treat dental conditions like periodontal disease. Some products make gum inflammation worse. Tartar and dental diseases require a dental procedure with general anesthesia at a veterinary clinic. When to Use Dental Products If your pet has smelly breath, visible tartar, bleeding gums, loose teeth, missing teeth, or signs of mouth pain, this is not the time to go shopping for dental products. This is the time to take your pet to the veterinarian and then schedule a dental procedure if your veterinarian recommends it. The time to start home dental care is when it will be effective and not painful for your pet, which means before your pet develops dental disease or after dental disease has been treated. It’s ideal to train puppies and kittens to have their teeth brushed while they’re young so they will build positive associations with dental care. If your pet has dental disease, talk to your veterinarian about the timing of home care; it’s usually best to start about a week after a dental procedure to give the gums time to heal. Active vs Passive Plaque Removal (How Much Work You Have to Do) Home plaque removal products fall into 2 categories: active and passive. With active plaque removal, the pet owner cleans the teeth with toothbrushes, toothpaste, or dental wipes. Passive plaque removal relies on chewing and doesn’t directly involve the pet owner; these are products like dental diets, treats, and chews. Many of us would love to use only passive dental care because tossing a treat to a dog is easier than brushing the dog’s teeth. (This is why the dental care aisle of the pet store has about 3 hooks for toothbrushes and 20 linear feet of toys and chews.) But passive dental care alone isn’t enough to keep a pet’s mouth healthy. Passive dental care products are best used along with professional cleanings when tooth brushing isn’t appropriate. Active plaque removal products have been shown to be most effective on the front teeth (the teeth the owner can easily reach). Passive plaque removal is generally most effective on the back teeth (the teeth used for chewing). Therefore, your veterinarian might recommend that you use more than one dental care product. Look for Veterinary Oral Health Council Seal Products that have the Veterinary Oral Health Council (VOHC) seal of acceptance have been shown to be effective for plaque or tartar control. The VOHC doesn’t test products; they review data submitted by product manufacturers. Some products that work, like most toothbrushes, haven’t been submitted to the VOHC, so lack of a seal doesn’t necessarily mean that a product is useless. However, looking for the VOHC seal is a good place to start. You can find lists of accepted products on the VOHC website: https://vohc.org/. Product Types Toothbrushes and toothpaste:
Dental rinses:
Dental chews, toys, diets, and treats:
Water additives:
Sources
Image source: https://www.pexels.com/photo/person-using-a-toothbrush-on-dog-with-shower-cap-4588018/ Laurie Anne Walden, DVM Photo by mahyar mirghasemi Photo by mahyar mirghasemi Dogs and cats need regular dental care, including thorough oral exams and dental cleanings. These procedures are best done under general anesthesia, but some pets don’t receive the dental care they need because their owners are worried about the safety of anesthesia. Most animals handle anesthesia well, though, and the risk is greatly reduced with preanesthetic testing, safe anesthetic drugs, and monitoring during the procedure. Reasons for Dental Anesthesia General anesthesia during a dental procedure allows for better medical care, reduces an animal’s stress and pain, and makes the procedure safer for everyone.
Anesthesia Safety Before an animal undergoes anesthesia, the benefits of the procedure are weighed against the possible risks. Although general anesthesia is safe overall, its risks range from minor drug effects that can be anticipated and managed to potentially fatal complications, which are rare. Animals receive a thorough physical exam before anesthesia and might also have preanesthetic laboratory tests. Preanesthetic tests are especially important for senior animals—the age group most often having dental procedures—because liver, kidney, and heart function all affect anesthesia risk. During the procedure, vital signs like heart rate, respiratory rate, blood oxygen saturation, and blood pressure are monitored. The patient’s level of anesthesia is also monitored and can be adjusted as needed. If your pet will be having anesthesia, tell the veterinarian all of the medications and supplements your pet is getting at home. Your veterinarian will also need to know if your pet has ever had problems with anesthesia in the past. If your pet has been to more than one clinic, be sure the anesthetizing veterinarian has your pet’s complete medical records and knows of any history of breathing trouble, heart conditions, seizures, or other medical problems. Problems With Anesthesia-Free Dental Scaling Some places offer dental scaling without anesthesia, but this procedure isn’t in an animal’s best interest.
Photo by mahyar mirghasemi on Unsplash Laurie Anne Walden, DVM Photo by Elena Mozhvilo Photo by Elena Mozhvilo Deciduous (baby) teeth that don’t fall out on their own are called persistent deciduous teeth. These extra teeth can cause problems if they are not removed surgically. Persistent deciduous teeth are most often seen in small-breed dogs and are uncommon in cats. Deciduous Teeth Like most mammals, dogs have 2 sets of teeth in their lifetime. Deciduous teeth erupt when puppies are a few weeks old and are replaced by permanent teeth from about 4 to 7 months of age. Dogs have 28 deciduous teeth and 42 permanent teeth. Deciduous teeth are able to fall out on their own because their roots gradually resorb (dissolve). Think of how children’s baby teeth look after they fall out: instead of long roots, they have jagged edges. Resorption of deciduous tooth roots is a complex process that is triggered, at least in part, by the pressure that erupting permanent teeth put on the deciduous tooth roots. As a permanent tooth starts to push toward the surface, the root of the deciduous tooth directly above it resorbs until the deciduous tooth falls away. The permanent tooth then emerges in the space left vacant by the deciduous tooth. Sometimes a permanent tooth isn’t in the right position under the gum, so the root of the deciduous tooth above it doesn’t resorb as it should. The permanent tooth then erupts next to the deciduous tooth, which stays in place as a persistent deciduous tooth. A common persistent deciduous tooth in dogs is the canine tooth, which is the long, sharpish tooth next to the incisors at the front of the mouth. Dogs with a persistent deciduous canine tooth have 2 canine teeth (1 deciduous and 1 permanent) right next to each other, usually touching. Problems Caused by Persistent Deciduous Teeth Two teeth crammed into a space meant for 1 tooth is never good. Overcrowding from a persistent deciduous tooth leads to a number of problems:
A permanent tooth that has been displaced by a persistent deciduous tooth is positioned incorrectly within the row of teeth. Displaced permanent teeth might be angled toward the lips or the tongue. A displaced lower canine tooth can hit the roof of the mouth when the mouth is closed. Diagnosis A persistent deciduous tooth is diagnosed when a deciduous tooth and the corresponding permanent tooth have both erupted but the deciduous tooth is still firmly fixed in place, not wiggly and getting ready to fall out. Dental radiographs are used to evaluate the tooth roots and look for other problems like impacted or missing teeth. Treatment A persistent deciduous tooth needs to be surgically removed as soon as it is diagnosed. The longer it stays in the mouth, the greater the risk of problems with the permanent tooth. If a persistent deciduous tooth is removed early, the permanent tooth will most likely move into the correct position on its own as the puppy grows. Photo by Elena Mozhvilo on Unsplash Laurie Anne Walden, DVM  Periodontal disease (disease of structures that support the teeth) is one of the most common medical problems of dogs and cats. This condition, which leads to bone loss around the tooth roots, causes the teeth to loosen and fall out. Although periodontal disease can be painful, animals often don’t show any outward symptoms until the disease is advanced. Periodontal disease may also increase the risk of heart, liver, and kidney problems. Regular dental care at home and periodic dental cleanings under anesthesia are the best ways to prevent periodontal disease. Causes Periodontal disease is caused by bacteria in the mouth—or more specifically, the body’s immune response to bacteria. Oral bacteria produce plaque, a sticky substance that coats the teeth. If not removed, plaque hardens into tartar. Bacteria, plaque, and tartar near the gumline activate the immune system, causing inflammation. The earliest stage of oral inflammation is gingivitis, or inflammation of the gums. Periodontal disease is more severe inflammation that affects the bone and other tissues around the tooth roots. Gingivitis is reversible with professional dental cleaning (including under the gums) and home dental care. Periodontal disease, which destroys the structures holding the teeth in place, is not reversible. The biggest risk factor for periodontal disease is the presence of plaque and tartar on the teeth. Other things that increase the risk are genetics, older age, crowded teeth, thin bone around the teeth (for example, in toy dog breeds), poor nutrition, and possibly medical conditions that reduce resistance to infection.[1] A study of 109 otherwise healthy cats found that all of them had some degree of periodontal inflammation.[2] Symptoms Dogs and cats can have remarkably bad dental disease without showing any symptoms of discomfort. Unpleasant mouth odor might be the only symptom that pet owners notice. Because periodontal disease affects the tooth roots, it’s hidden from view in the early stages. It’s more obvious once bone has been lost to the point that the tooth roots are exposed or teeth start falling out. The symptoms, if any, begin with symptoms of gingivitis and get worse as the inflammation becomes more severe:
Diagnosis Very advanced periodontal disease causes changes that can be seen on oral examination of an awake animal. Diagnosing earlier stages and assessing the extent of the disease require examination with the animal under anesthesia. The diagnosis is made by examining the entire mouth, probing the gums to find pockets of inflammation/infection, and taking dental radiographs (if available) to get a look at the tooth roots and the surrounding bone. Treatment and Prevention Gingivitis and early stages of periodontal disease are managed with dental cleaning under anesthesia followed by home dental care. Anesthesia is necessary because plaque and tartar must be removed from the parts of the teeth under the gums. Scraping tartar off the teeth of an awake animal is not enough. It makes the teeth look better, but it does nothing to treat the real problem and can make things worse by delaying a more thorough cleaning. Teeth with later stages of periodontal disease are treated surgically. The procedure used depends on the stage of disease and the condition of the bone. Sometimes a tooth can be saved with an endodontic procedure like a root canal, but in many cases extraction of the tooth is the best option. Plaque starts to form on teeth again soon after a dental cleaning, so regular home dental care is ideal. Brushing the teeth with pet (not human) toothpaste is the standard of care for animals that allow it. Many other products to help remove dental plaque are available. See the blog post on dental home care for some ideas and talk to your veterinarian about products that would work for your pet. References 1. Wallis C, Holcombe LJ. A review of the frequency and impact of periodontal disease in dogs. J Small Anim Pract. 2020;61(9):529-540. doi: 10.1111/jsap.13218 2. Girard N, Servet E, Biourge V, Hennet P. Periodontal health status in a colony of 109 cats. J Vet Dent. 2009;26(3):147-155. doi: 10.1177/089875640902600301 Photo by Chris Smith Laurie Anne Walden, DVM 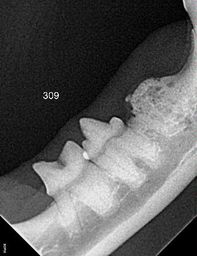 Radiograph of 3 cat teeth undergoing resorption. Tooth on the far right is in an advanced stage of resorption. Image by Rebecca Johnson, DVM. Radiograph of 3 cat teeth undergoing resorption. Tooth on the far right is in an advanced stage of resorption. Image by Rebecca Johnson, DVM. Tooth resorption is a potentially painful dental problem that is common in adult cats and occasionally affects dogs. The condition gets worse over time and can involve many teeth or only a single tooth root. Animals with tooth resorption and mouth pain might not have any obvious symptoms. Description Tooth resorption is the process of tooth breakdown and reabsorption by the body. Tooth root resorption is normal in baby teeth. Think of how a baby tooth looks after it falls out: it has a jagged edge instead of long roots. Its roots were resorbed as the permanent tooth moved into its place. If its roots had not been resorbed, the baby tooth would stay in the mouth instead of falling out to make room for the permanent tooth. For reasons that are still unclear, many cats experience abnormal resorption of adult teeth. Resorption of adult teeth can affect only the roots or both the roots and the crown (the visible part of the tooth above the gumline). Resorption is not the same as cavities, which are rare in cats and dogs. Tooth resorption in adult teeth usually begins with the loss of a small amount of the hard outer tooth surface at or below the gumline. Resorption progresses until it reaches the soft pulp at the center of the tooth. Another type of tooth resorption begins in the pulp and works its way outward.[1] The process involves bone remodeling along with tooth destruction, and in the final stage the root mostly disappears and is replaced with bone.[2] Inflammation plays a part in tooth resorption, although whether inflammation causes resorption or resorption causes inflammation is not known.[3] In any case, many cats with tooth resorption also have gingivitis or more severe inflammation in the mouth. Whether tooth resorption is painful depends on the degree of inflammation, location of the resorbed area (above or below the gumline), stage of resorption, and presence of other problems like infection. Symptoms Tooth resorption is very often a hidden condition that isn’t found until a cat is under anesthesia for a dental procedure and has dental radiographs (x-ray images) taken. Cats and dogs can have mouth pain with very subtle or no symptoms of discomfort. Gingivitis is sometimes a sign of underlying tooth resorption. Animals with tooth resorption might have these symptoms:
Diagnosis Tooth resorption is diagnosed with dental imaging (radiographs or computed tomography) and a full oral examination that includes probing around all sides of the teeth. These procedures require general anesthesia or at least deep sedation. Examination of a cooperative awake patient can reveal resorption that affects the crown, but it won’t show resorption of tooth roots. Treatment Currently the only effective treatment for tooth resorption is extraction of the affected teeth. If the tooth roots have already been replaced by bone, only the crown of the tooth might need to be removed. Decisions about whether to extract, when to extract, and how much tooth to extract are based on how the teeth look on radiographs and whether the condition is likely to be painful.[3] Medical treatments like antibiotics and steroids don’t stop tooth resorption. Tooth resorption can’t be prevented because the cause isn’t known.[2] The best way to catch the problem is with regular dental care, including an oral examination and radiographs under anesthesia as recommended by a veterinarian. References 1. AVDC nomenclature: tooth resorption. American Veterinary Dental College website. https://avdc.org/avdc-nomenclature/. Accessed January 31, 2020. 2. Reiter AM. Tooth resorption in small animals. Merck Veterinary Manual website. https://www.merckvetmanual.com/digestive-system/dentistry/tooth-resorption-in-small-animals. Updated May 2014. Accessed January 31, 2020. 3. Smith MM. Tooth resorption in cats: don’t think you know; know you know! In: VMX 2020 Proceedings: Small Animal & Exotics, Book 1. Orlando, FL: North American Veterinary Community; 2020. Laurie Anne Walden, DVM Tooth root abscesses are painful and need prompt treatment, but the signs can be easy to miss. Dogs don’t always show that their mouths hurt, and tooth abscesses can mimic other conditions.
Causes Tooth root abscesses are pockets of pus caused by bacteria that invade the deep structures of the tooth. They often occur in teeth with severe periodontal disease or gingivitis (gum disease), especially if the gum has receded around the tooth. Teeth that are cracked or fractured are also at risk for root abscesses. Teeth can fracture when a dog chews on something hard, like a bone, cow hoof, ice cube, hard nylon toy, or rock. Fractures that expose the pulp cavity (the inner part of the tooth) give bacteria a route to the tooth root. Affected teeth The upper fourth premolar—the large cheek tooth on each side of the upper jaw—is a common site of root abscess. This tooth, also called the carnassial tooth, is used to crush food. When a dog crunches something hard, a carnassial tooth can sustain a slab fracture (shearing off a slab from the side of the tooth) or can crack down the center. The roots of the carnassial tooth reach nearly to the eye, so an abscessed root causes swelling just below the eye. Root abscesses can occur in any tooth. The large canine (fang) teeth are frequently broken and are also common sites of root abscesses. Symptoms Although tooth root abscesses are very painful, dogs’ signs of mouth pain can be subtle. Some dogs don’t show any symptoms at all. Signs of a tooth root abscess can include the following:
A veterinarian may be able to find evidence of a tooth root abscess during examination of an awake patient. However, dogs with tooth root abscesses sometimes have too much mouth pain to allow much of an oral examination without sedation. Diagnosis often requires dental radiographs (x-ray images) or at least a full oral examination with the patient under anesthesia. Dental radiographs sometimes reveal tooth root abscesses that can’t be seen any other way. Treatment Untreated tooth root abscesses cause prolonged pain and tooth loss. The infection can spread to other tooth roots and to the face, potentially even affecting the eye. Dogs with tooth root abscesses need antibiotics and pain relief. The source of the infection must also be removed. There are 2 options for treating an abscessed tooth root:
If you think your dog might have a tooth root abscess, make an appointment with your veterinarian as soon as possible. Your veterinarian will examine your dog and, if the signs indicate an abscess, will probably prescribe an antibiotic and an analgesic (pain reliever). The next step will be either another appointment with your veterinarian for tooth extraction or referral to a dental specialist for possible root canal therapy. Both extraction and root canal therapy require general anesthesia. If you would like your dog to keep his tooth, root canal treatment is the best option. Antibiotics alone are rarely enough to treat a root abscess. However, not all teeth are candidates for root canal therapy. The dental specialist will evaluate dental radiographs to see if root canal treatment is a good option and will extract the tooth if necessary. Prevention Sometimes tooth root abscesses are unavoidable. But you can take some measures to reduce your dog’s risk:
Laurie Anne Walden, DVM  Dental radiography (x-ray imaging) is an important diagnostic tool for pets, just as it is for people. Animals don’t always show signs of mouth pain, and radiographs may be the only way to know there’s a problem. Most dental disease in dogs and cats happens under the gumline, where it’s hidden from view. In published studies, radiographs revealed disease in apparently healthy teeth in 27.8% of dogs and 41.7% of cats. Dental radiographs find problems that can’t always be seen on a physical examination:
Radiographs also guide dental procedures in pets. For example, some dog and cat teeth have curved roots, extra roots, or roots that extend very close to the jawbone. It’s best to know about these issues before trying to extract these teeth. In animals, dental radiography requires general anesthesia or sedation. The radiographs use sensors or small film cassettes placed inside the mouth, and animals can’t wiggle during the procedure. Imagine putting an x-ray sensor between your dog’s teeth and politely asking her to lie still and not chew on it. Now imagine asking your cat the same thing. Dental radiographs are often obtained while a pet is already under anesthesia for a dental procedure. Dental radiography delivers a very small radiation dose to the patient. The American Veterinary Dental College reports that “the radiation risk to the patient from taking dental radiographs is minimal.” Like people, pets benefit from having full-mouth dental radiography from time to time to be sure no problems are lurking under the surface. Oral imaging may also be indicated in pets with these conditions:
Photo by muhannad alatawi Laurie Anne Walden, DVM  Have you wondered what happens during a dental cleaning at the veterinary hospital? Recently I brought my dog Oreo to the clinic to clean her teeth. Read on to see what was involved. Oreo is about 7 years old and had her last dental cleaning 2 years ago. I’ve brushed her teeth at home, but not regularly enough to keep tartar from building up. 1. Preliminaries Oreo came to the clinic with an empty stomach. Thoroughly cleaning pets’ teeth requires general anesthesia, so Oreo had bloodwork to check for abnormalities that might affect the anesthetic plan. The analysis included blood cell counts, markers of liver and kidney function, electrolyte levels, blood sugar level, and other tests. I also gave her a complete physical exam. In the coming months Mallard Creek will be installing a dental x-ray unit, which will let us further assess patients before their dental procedures. [Updated: Mallard Creek Animal Hospital began including dental x-ray imaging with dental procedures in March 2018.] 2. Preanesthetic medication Oreo received a sedative injection before going under general anesthesia. This sedative reduced the amount of general anesthetic she needed. Injected sedatives wear off more slowly than the general anesthetic agents we use at Mallard Creek, so Oreo was a little sleepy for a few hours after her procedure. 3. Intravenous catheter We clipped fur from Oreo’s front leg, cleaned the skin with an antiseptic, and placed a catheter in her vein. During the procedure, Oreo received intravenous fluids through the catheter. 4. Anesthesia induction and endotracheal tube placement Oreo’s general anesthesia began with an injection of a fast-acting anesthetic agent through her catheter. Once she was asleep, we placed an endotracheal tube in her trachea (windpipe). This tube allowed us to deliver oxygen and anesthetic gas to keep her asleep. An inflatable cuff on the tube also kept water and debris out of her lungs. 5. Monitoring Pam, one of our trained veterinary technicians, looked after Oreo while I was cleaning her teeth. Pam monitored Oreo’s heart rate, breathing, blood oxygen level, and level of anesthesia. 6. Tooth scaling I removed plaque and tartar from Oreo’s teeth with an ultrasonic scaler. This instrument vibrates at a very high speed to remove tartar quickly and efficiently. It sprays water while it’s cleaning to keep the scaler tip cool. Because Oreo was under anesthesia, I was able to remove plaque and tartar under her gums, which is essential to prevent gingivitis and periodontal disease. Oreo’s gums bled a little during scaling, showing that she had already developed some gingivitis even though her gums did not look particularly inflamed on the physical exam. 7. Tooth polishing After I scaled Oreo’s teeth, I polished them with polishing compound. The point of polishing is not to make the teeth look pretty. Polishing smooths the tooth enamel after scaling, removing tiny grooves where bacteria and plaque can take hold. Brushing with toothpaste does not have the same effect. 8. Rinse and repeat After I rinsed the polishing compound from Oreo’s teeth, Pam and I turned her over to repeat the process on the other side. 9. Waking up When the cleaning was finished, Pam turned off the anesthetic gas and let Oreo breathe oxygen. During this time, Pam continued to monitor Oreo’s vital signs and trimmed her toenails. After a few minutes, Oreo began waking up, and Pam removed her endotracheal tube. Later on, Pam removed the intravenous catheter. 10. Going home Oreo came home with a bandage on her front leg where the catheter had been. I removed the bandage that evening. After a couple of days it was time to restart her home dental care! Laurie Anne Walden, DVM Dental disease is very common in dogs and cats. Luckily, home dental care can help prevent painful tooth and gum conditions. Dogs and cats rarely get cavities. However, just like people, they develop gingivitis (inflammation of the gums) and periodontal disease (inflammation and infection of the structures that hold the teeth in place). According to the American Veterinary Dental College, periodontal disease is the most common disease diagnosed in adult dogs and cats. It causes bad breath, mouth pain, and tooth loss. It's also associated with heart, kidney, and liver problems. Because periodontal disease occurs under the gumline, you might not know your pet has the condition until it's advanced. Pets with unstained teeth and little tartar buildup can still have periodontal disease. The best way to prevent periodontal disease is to remove plaque daily at home and have the teeth professionally cleaned from time to time, just as you do with your own teeth. Professional dental cleanings for pets are performed under general anesthesia to allow removal of plaque and bacteria under the gums. (Simply scraping tartar off the visible tooth surfaces doesn't prevent gum disease.) Home dental care products If your pet has mouth pain or is bleeding from the gums, consult a veterinarian before beginning a home dental care program. Plaque removal can be painful for animals with existing oral disease unless it's done under anesthesia. When you're choosing oral hygiene products, look for the Veterinary Oral Health Council (VOHC) seal on the product packaging. The VOHC seal means that the product meets standards for effectiveness against plaque, tartar, or both. You can find lists of accepted products on the VOHC website. Tooth brushing is the standard way to remove plaque at home. Brushing daily or every other day has been shown to be significantly more effective than brushing once a week.[1] Use toothpaste formulated for pets, not for humans; it's safer for them to swallow. Here are two videos explaining the procedure in detail:
Medicated dental wipes are an alternative to toothbrushes. In addition to providing mechanical plaque removal, these products contain agents that slow plaque buildup. Oral dental gels contain antibacterial ingredients that improve breath odor and decrease plaque formation. If your reaction at this point is "I'm liable to lose a finger if I try to stick something in my pet's mouth," there are other options. Indirect dental care products can be reasonable alternatives, especially for animals that might bite. Dental diets are designed to abrade tooth surfaces during chewing. They work only on teeth in contact with the food. Dental chews and treats also mechanically remove plaque or tartar from teeth that they contact. Some chews are made of rawhide; others are soluble. Be aware that any of these products can pose a choking risk. Rigid products (like bones or hard nylon) may fracture teeth. Dr. Jan Bellows, a veterinary dental specialist, recommends these precautions[1]:
Water additives accepted by the VOHC inhibit the growth of bacteria in the mouth and reduce plaque and tartar buildup. Your pet doesn't have to have bad breath! Call the clinic if you have any questions about your pet's oral health. References 1. Harvey C, Serfilippi L, Barnvos D. Effect of frequency of brushing teeth on plaque and calculus accumulation, and gingivitis in dogs. J Vet Dent. 2015;32(1):16-21. doi:10.1177/089875641503200102 2. Bellows J. The ultimate guide to veterinary dental home care. DVM360. May 4, 2017. Accessed February 5, 2021. https://www.dvm360.com/view/ultimate-guide-veterinary-dental-home-care Photo by Ryan McGuire |
AuthorLaurie Anne Walden, DVM Categories
All
Archives
June 2024
The contents of this blog are for information only and should not substitute for advice from a veterinarian who has examined the animal. All blog content is copyrighted by Mallard Creek Animal Hospital and may not be copied, reproduced, transmitted, or distributed without permission.
|
- Home
- About
- Our Services
- Our Team
-
Client Education Center
- AKC: Spaying and Neutering your Puppy
- Animal Poison Control
- ASPCA Poisonous Plants
- AVMA: Spaying and Neutering your pet
- Biting Puppies
- Boarding Your Dog
- Caring for the Senior Cat
- Cats and Claws
- FDA warning - Bone treats
- Force Free Alliance of Charlotte Trainers
- Getting your Cat to the Vet - AAFP
- Holiday Hazards
- How To Feed Cats for Good Health
- How to Get the Most Out of your Annual Exam
- Indoor Cat Initiative - OSU
- Introducing Your Dog to Your Baby
- Moving Your Cat to a New Home
- Muzzle Training
- Osteoarthritis Checklist for Cats
- What To Do When You Find a Stray
- Our Online Store
- Dr. Walden's Blog
- Client Center
- Contact
- Cat Enrichment Month 2024
|
Office Hours
Monday through Friday 7:30 am to 6:00 pm
|
Mallard Creek Animal Hospital
2110 Ben Craig Dr. Suite 100
|
Site powered by Weebly. Managed by IDEXX Laboratories


 RSS Feed
RSS Feed