Laurie Anne Walden, DVM  Mast cell tumors are common in dogs and somewhat common in cats. In dogs, mast cell tumors are usually lumps on or under the skin. Mast cell tumors in cats can affect the skin or the internal organs.[1] Mast cells are a normal part of the immune system. They are most often found in the skin, digestive tract, and other areas that are exposed to substances from the environment. Mast cells are full of granules that contain histamine and other chemicals that are released as part of allergic and inflammatory responses. You’ve seen mast cells in action yourself: the itchy lump you get after a mosquito bite is caused by mast cells in the skin releasing histamine and other substances. Mast cell tumors are cancerous growths made up of mast cells. Signs in Dogs Mast cell tumors are most common in older dogs but occur in dogs of all ages. Dogs of any breed can develop mast cell tumors. Breeds at higher risk than others include retrievers, shar-peis, and brachycephalic (flat-faced) breeds like boxers, pugs, and Boston terriers. In dogs, mast cell tumors can look similar to other conditions. Some look and feel just like benign fatty lumps. Mast cell tumors in dogs vary in appearance and behavior. A mast cell tumor might be a smooth, round, raised skin lump; a red, itchy lump; or a soft lump under the skin. Some are solitary growths, and some are clusters of lumps or small bumps. Some grow very slowly, with no apparent change for months; others grow quickly. Mast cell tumors sometimes get bigger (or pinker or itchier) and then return to their normal appearance. This change happens when they release histamine. More serious effects of histamine release include decreased appetite, vomiting, diarrhea, blood in the stool, and collapse.[1,2] Signs in Cats Most cats with mast cell tumors are older, although an atypical form is most common in young cats. Siamese may be more likely than other cat breeds to have mast cell tumors.[3] In cats, the signs of mast cell tumors depend on their location (skin or internal organs) and the tumor subtype, which determines how aggressive they are. As in dogs, mast cell tumors in cats can mimic other conditions and do not all look and behave the same way. Mast cell tumors in the skin can be smooth, round growths or flat red patches, and they might grow quickly or very slowly. Mast cell tumors inside the body most often affect the spleen or digestive tract and can cause decreased activity, decreased appetite, vomiting, diarrhea, and other general signs of illness.[1,3] Diagnosis Most mast cell tumors of the skin can be diagnosed during a veterinary appointment with a needle aspirate, in which a small sample of cells is removed with a needle and syringe and examined under a microscope. Because putting a needle in a mast cell tumor can cause histamine release, veterinarians often give an antihistamine when they aspirate a mast cell tumor. A needle aspirate can show that a patient has a mast cell tumor, but it doesn’t give enough information to know the prognosis. Some mast cell tumors are single lumps that don’t spread to lymph nodes or distant parts of the body. Others are more invasive and have a high risk of spreading through the body. Currently the only way to know the grade or type of a mast cell tumor, and hence the prognosis, is by surgically removing all or part of the tumor and sending this biopsy sample to a laboratory for analysis. Patients with high-grade or aggressive mast cell tumors, including cats with mast cell tumors in internal organs, benefit from further tests to find out whether the cancer has spread or is causing other problems. This workup can include blood and urine tests, lymph node aspiration, imaging (such as ultrasound or computed tomography), and bone marrow analysis. Whether to do these tests before or after biopsy depends on the patient and the tumor. Treatment Surgical removal is recommended for most mast cell tumors and might be the only treatment (other than antihistamines) needed for low-grade mast cell tumors of the skin. Cancerous mast cells extend past the edges of the visible lump, so a wide area of normal-appearing skin around the tumor must be removed. The biopsy report indicates whether all of the tumor was removed during the procedure. Chemotherapy, other medications, and radiation therapy are available for patients with aggressive tumors, cancer in internal organs, tumors in areas where wide removal isn’t possible, or tumors that aren’t completely removed during surgery. Your veterinarian is likely to recommend referral to an oncologist if your pet might need these types of treatment. Prognosis The prognosis is good for patients with mast cell tumors that haven’t spread and are completely removed with surgery, radiation therapy, or both. These patients sometimes develop another mast cell tumor later, so all new lumps warrant a visit to the veterinarian. For patients with other types of mast cell tumor, the prognosis depends on tumor grade, location, and response to treatment. References 1. Blackwood L, Murphy S, Buracco P, et al. European consensus document on mast cell tumours in dogs and cats. Vet Comp Oncol. 2012;10(3):e1-e29. doi:10.1111/j.1476-5829.2012.00341.x 2. Couto CG. Mast cell tumors: to cut or not to cut. Paper presented at: 2018 Michigan Veterinary Conference; January 26-28, 2018; Lansing, Michigan. Accessed February 14, 2020. https://www.michvma.org/resources/Documents/MVC/2018%20Proceedings/couto_04.pdf 3. Henry C, Herrera C. Mast cell tumors in cats: clinical update and possible new treatment avenues. J Feline Med Surg. 2013;15(1):41-47. Photo by JC Gellidon
0 Comments
Laurie Anne Walden, DVM 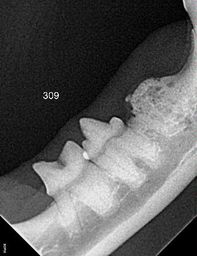 Radiograph of 3 cat teeth undergoing resorption. Tooth on the far right is in an advanced stage of resorption. Image by Rebecca Johnson, DVM. Radiograph of 3 cat teeth undergoing resorption. Tooth on the far right is in an advanced stage of resorption. Image by Rebecca Johnson, DVM. Tooth resorption is a potentially painful dental problem that is common in adult cats and occasionally affects dogs. The condition gets worse over time and can involve many teeth or only a single tooth root. Animals with tooth resorption and mouth pain might not have any obvious symptoms. Description Tooth resorption is the process of tooth breakdown and reabsorption by the body. Tooth root resorption is normal in baby teeth. Think of how a baby tooth looks after it falls out: it has a jagged edge instead of long roots. Its roots were resorbed as the permanent tooth moved into its place. If its roots had not been resorbed, the baby tooth would stay in the mouth instead of falling out to make room for the permanent tooth. For reasons that are still unclear, many cats experience abnormal resorption of adult teeth. Resorption of adult teeth can affect only the roots or both the roots and the crown (the visible part of the tooth above the gumline). Resorption is not the same as cavities, which are rare in cats and dogs. Tooth resorption in adult teeth usually begins with the loss of a small amount of the hard outer tooth surface at or below the gumline. Resorption progresses until it reaches the soft pulp at the center of the tooth. Another type of tooth resorption begins in the pulp and works its way outward.[1] The process involves bone remodeling along with tooth destruction, and in the final stage the root mostly disappears and is replaced with bone.[2] Inflammation plays a part in tooth resorption, although whether inflammation causes resorption or resorption causes inflammation is not known.[3] In any case, many cats with tooth resorption also have gingivitis or more severe inflammation in the mouth. Whether tooth resorption is painful depends on the degree of inflammation, location of the resorbed area (above or below the gumline), stage of resorption, and presence of other problems like infection. Symptoms Tooth resorption is very often a hidden condition that isn’t found until a cat is under anesthesia for a dental procedure and has dental radiographs (x-ray images) taken. Cats and dogs can have mouth pain with very subtle or no symptoms of discomfort. Gingivitis is sometimes a sign of underlying tooth resorption. Animals with tooth resorption might have these symptoms:
Diagnosis Tooth resorption is diagnosed with dental imaging (radiographs or computed tomography) and a full oral examination that includes probing around all sides of the teeth. These procedures require general anesthesia or at least deep sedation. Examination of a cooperative awake patient can reveal resorption that affects the crown, but it won’t show resorption of tooth roots. Treatment Currently the only effective treatment for tooth resorption is extraction of the affected teeth. If the tooth roots have already been replaced by bone, only the crown of the tooth might need to be removed. Decisions about whether to extract, when to extract, and how much tooth to extract are based on how the teeth look on radiographs and whether the condition is likely to be painful.[3] Medical treatments like antibiotics and steroids don’t stop tooth resorption. Tooth resorption can’t be prevented because the cause isn’t known.[2] The best way to catch the problem is with regular dental care, including an oral examination and radiographs under anesthesia as recommended by a veterinarian. References 1. AVDC nomenclature: tooth resorption. American Veterinary Dental College website. https://avdc.org/avdc-nomenclature/. Accessed January 31, 2020. 2. Reiter AM. Tooth resorption in small animals. Merck Veterinary Manual website. https://www.merckvetmanual.com/digestive-system/dentistry/tooth-resorption-in-small-animals. Updated May 2014. Accessed January 31, 2020. 3. Smith MM. Tooth resorption in cats: don’t think you know; know you know! In: VMX 2020 Proceedings: Small Animal & Exotics, Book 1. Orlando, FL: North American Veterinary Community; 2020. |
AuthorLaurie Anne Walden, DVM Categories
All
Archives
June 2024
The contents of this blog are for information only and should not substitute for advice from a veterinarian who has examined the animal. All blog content is copyrighted by Mallard Creek Animal Hospital and may not be copied, reproduced, transmitted, or distributed without permission.
|
- Home
- About
- Our Services
- Our Team
-
Client Education Center
- AKC: Spaying and Neutering your Puppy
- Animal Poison Control
- ASPCA Poisonous Plants
- AVMA: Spaying and Neutering your pet
- Biting Puppies
- Boarding Your Dog
- Caring for the Senior Cat
- Cats and Claws
- FDA warning - Bone treats
- Force Free Alliance of Charlotte Trainers
- Getting your Cat to the Vet - AAFP
- Holiday Hazards
- How To Feed Cats for Good Health
- How to Get the Most Out of your Annual Exam
- Indoor Cat Initiative - OSU
- Introducing Your Dog to Your Baby
- Moving Your Cat to a New Home
- Muzzle Training
- Osteoarthritis Checklist for Cats
- What To Do When You Find a Stray
- Our Online Store
- Dr. Walden's Blog
- Client Center
- Contact
- Cat Enrichment Month 2024
|
Office Hours
Monday through Friday 7:30 am to 6:00 pm
|
Mallard Creek Animal Hospital
2110 Ben Craig Dr. Suite 100
|
Site powered by Weebly. Managed by IDEXX Laboratories

 RSS Feed
RSS Feed